World Backup Day highlights the importance of protecting data – but in healthcare, having data copies alone does not ensure systems can be restored when they fail.
Most healthcare organizations rely on successful backup reports as proof of protection. However, this creates a gap between data being stored and systems being recoverable under real conditions.
- A backup confirms data exists
- Recovery determines whether operations can continue
- Patient care depends on system availability—not just stored data

Having the data is only half the battle; ensuring it works for clinical care is the goal.
Research shows that only 54% of organizations regularly test their recovery processes, meaning many healthcare providers may not know if their systems will actually work during an incident. (Source)
In environments where EHR systems, imaging platforms, and clinical workflows are interconnected, failure is not just about data loss—it’s about operational disruption and delayed care.
👉 This raises a critical question: Are healthcare organizations truly protected—or just assuming they are?
Why World Backup Day Can Create a False Sense of Security?
World Backup Day raises awareness about data protection, but healthcare environments require a deeper focus on recovery outcomes.
What Healthcare organizations assume is “covered”
Most healthcare teams equate a successful backup status with protection.
Typical assumptions:
- Data is safe
- Systems can be restored anytime
- Operations will resume quickly
These assumptions are based on storage confirmation—not recovery validation.
Why successful data copies don’t reflect real outcomes
A completed backup only confirms that data was written to a storage location. It does not confirm:
- data integrity
- system compatibility
- recovery speed
- application functionality
This gap is widespread. This creates a disconnect between:
- reported success (backup completed)
- actual readiness (systems restorable under pressure)
For a deeper look at how recovery validation works in practice, see our validated recovery process
The gap between stored information and usable systems
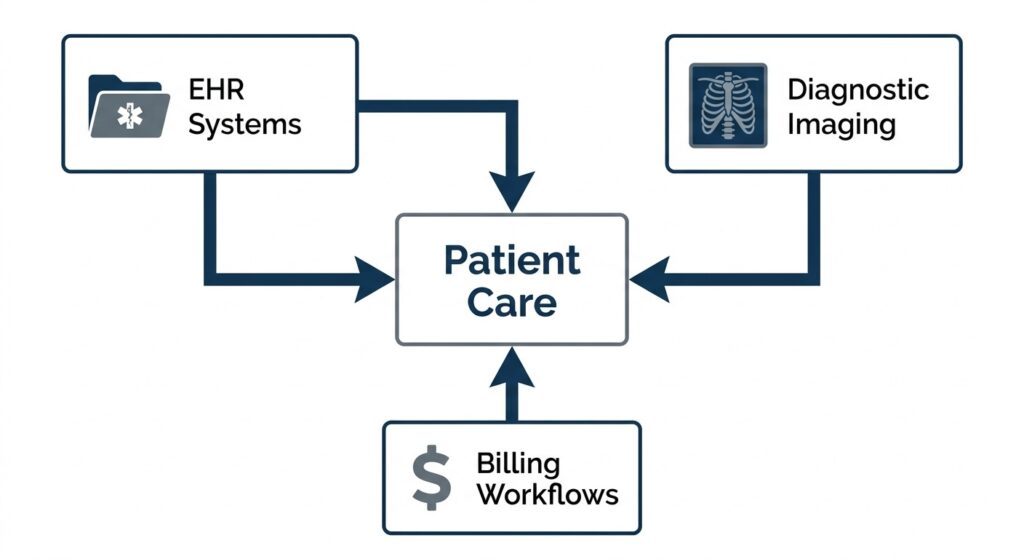
Recovery fails if system dependencies are not accounted for.
Healthcare environments depend on interconnected systems:
- EHR platforms
- imaging systems
- scheduling and billing workflows
Even if raw data exists, recovery fails if:
- dependencies are missing
- configurations are incomplete
- data states are inconsistent
Result: Systems may “recover” technically but remain unusable operationally
If assumptions don’t hold during an incident, the impact becomes visible immediately—especially when clinical systems stop functioning.
What Really Happens When Clinical Systems Fail
When systems fail, the impact extends beyond IT into clinical operations and patient care.
Impact on patient care and operations
When clinical systems fail, the issue is not limited to data access—it disrupts the entire care delivery process.
Affected areas include:
- patient records (EHR systems)
- diagnostic imaging
- appointment scheduling
- billing and coordination workflows
This leads to delayed treatments, manual workarounds and reduced care efficiency
Delays, disruptions, and system dependencies
Healthcare systems operate as interconnected environments, not isolated tools.
A failure in one system can:
- block access across multiple platforms
- break workflow continuity
- delay clinical decision-making
Even if data exists, dependencies between systems prevent immediate usability.
Why recovery speed defines outcomes
Recovery is not binary (working vs not working). It is measured by:
- how fast systems are restored
- whether data is usable immediately
- whether workflows resume without disruption
Industry estimates show that IT downtime can cost thousands per minute, but in healthcare the cost extends to operational disruption and patient risk. [source]
This shifts the priority from:
- storing data → restoring systems quickly and reliably
If system recovery is slow, incomplete, or inconsistent, the issue is often not the absence of data—but the inability to use it effectively.
Identify Why Stored Data Fails During Recovery
Failures during recovery are often caused by issues that remain hidden during normal operations.
Hidden corruption and incomplete states
Stored data can appear intact but still be unusable.
Common issues include:
- incomplete data snapshots
- corrupted files within datasets
- missing system configurations
These issues are often undetected until recovery is attempted.
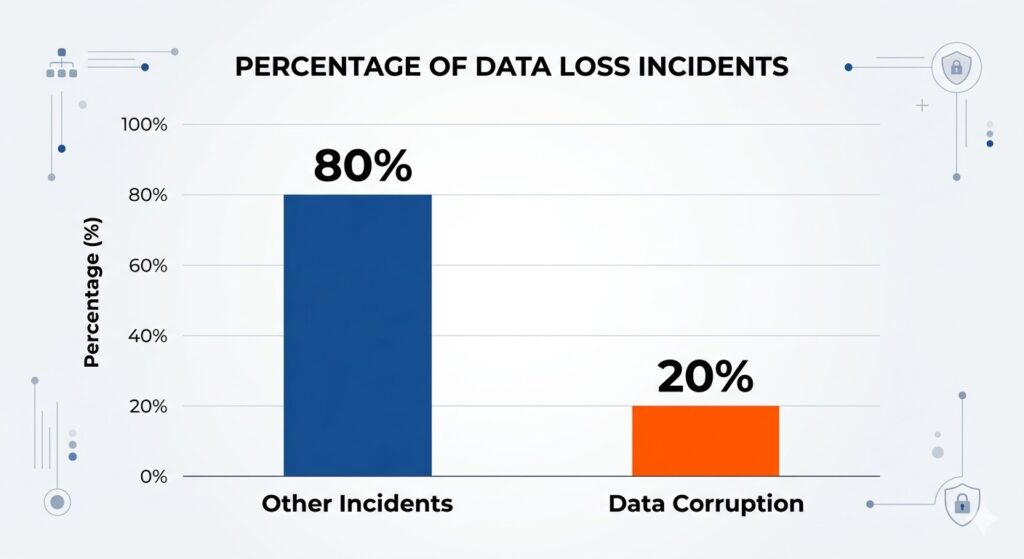
Moving from assumed resilience to proven readiness requires measurable validation.
Industry research indicates that data corruption contributes to nearly 20% of data loss incidents, making it a frequent but overlooked failure point. [source]
Reinfection risks from compromised environments
In ransomware scenarios, attackers increasingly target not just production systems—but also stored data.
This means:
- backup environments may already be compromised
- restored data may reintroduce threats
- recovery can fail even when data is available
Without isolation and validation, recovery can recreate the same failure conditions. For deeper context on this risk, see our post – clean and usable restore points
Lack of restore validation
The most critical failure point is not storage – it is lack of testing.
- Many organizations do not simulate real recovery scenarios
- Recovery steps are unverified until an actual incident
- System dependencies are not validated in advance
This highlights a consistent issue: Data may exist—but recovery outcomes remain uncertain
These failures point to a larger issue – not the absence of data, but the gap between storing information and restoring full operations.
Define “Recovery-Ready” Healthcare Systems
Recovery readiness is achieved only when systems can be restored predictably under real conditions.
Verified restore processes
Recovery readiness starts with proven outcomes, not assumptions. This requires:
- testing full system restoration (not just files)
- validating application functionality post-restore
- confirming workflows operate as expected
Without verification, recovery remains theoretical. For a detailed approach to validation, check our validated recovery process
Clean and uncompromised data
Recovery must ensure that restored data is:
- free from corruption
- isolated from prior compromise
- consistent across systems
This is critical in ransomware scenarios, where restoring compromised data can reintroduce the same issue. Recovery success depends on data integrity, not just availability
Tested recovery timelines
Recovery readiness includes knowing:
- how long restoration will take
- which systems recover first
- how dependencies affect timelines
Without this clarity, downtime becomes unpredictable and operations remain disrupted longer than expected.
Reliable recovery requires predictable and tested timelines
If recovery readiness depends on proven outcomes, the next step is asking the right question – one that goes beyond basic assumptions.
Ask the Right Recovery Question on March 31
The value of World Backup Day depends on asking the right operational question.
Moving beyond “Are we backed up?”
World Backup Day encourages a simple question:
Is our data backed up?
In healthcare, this is insufficient.
A more relevant question is:
Can we restore clinical systems quickly, cleanly, and without risk?
Because protection is not defined by storage – it is defined by outcome under failure conditions.
Evaluating real readiness under pressure
During an actual incident, recovery must deliver:
- immediate access to accurate patient data
- functional clinical systems (EHR, imaging, workflows)
- minimal disruption to care delivery
This requires:
- validated recovery processes
- known recovery timelines
- confidence in system integrity
Without these, organizations operate with assumed resilience, not proven readiness.
Identifying hidden risks before an incident
Common gaps that remain undetected:
- no full-system recovery testing
- unknown system dependencies
- reliance on unverified data states
These risks only surface during real failures—when time is limited and impact is immediate.
This is where most organizations shift from:
confidence → uncertainty
Understanding the right question is only useful if it leads to measurable insight into your current environment.
Assess Current Recovery Risk in Healthcare Systems
Understanding risk exposure is the first step toward improving recovery reliability.
Indicators of recovery gaps
Recovery risks are often hidden until systems fail. Key indicators include:
- backups completed but never tested in full-system scenarios
- unclear or inconsistent recovery timelines
- inability to restore dependent systems together
These signals point to unverified recovery capability, not confirmed resilience.
Common blind spots in healthcare environments
Healthcare organizations frequently operate with:
- reliance on storage success instead of recovery validation
- limited visibility into system dependencies (EHR, imaging, workflows)
- absence of isolated, clean recovery points
These gaps increase the likelihood of extended downtime, failed or repeated recovery attempts and disruption to clinical operations
How to validate readiness with confidence
Recovery readiness requires measurable validation:
- test full-system restoration (not partial data)
- confirm data integrity and usability post-restore
- establish predictable recovery timelines
Without this, organizations cannot determine whether systems will function under real conditions. Start with a structured evaluation of your current environment
World Backup Day raises awareness about protecting data. But in healthcare, resilience depends on one outcome:
Whether systems can be restored reliably when it matters most.
Answer Key Questions on Healthcare Data Recovery
What is World Backup Day in healthcare?
World Backup Day promotes data protection awareness. In healthcare, it emphasizes system recovery capability, ensuring clinical systems restore quickly and safely—not just storing data.
Why are backups not enough for healthcare systems?
Backups store data but do not ensure system functionality, recovery speed, or operational continuity. Healthcare systems require full restoration of clinical workflows, not just access to stored data.
What is the biggest risk with untested backups?
Untested backups fail during recovery due to corruption, missing dependencies, or misconfiguration.
How does downtime affect healthcare operations?
Downtime disrupts patient care, clinical workflows, and system access. It delays treatment, reduces efficiency, and impacts operational continuity across healthcare environments.
What defines recovery readiness in healthcare?
Recovery readiness ensures systems restore quickly, with clean data, and full functionality. It requires validated recovery processes, tested timelines, and confirmed system integrity.
Last updated on April 9, 2026




